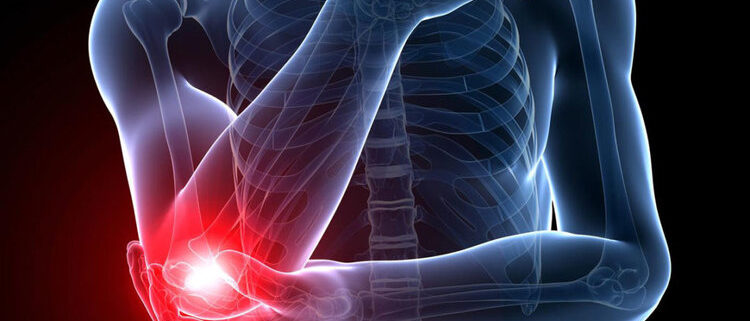
Epicondylitis: When the elbow hurts!
''I have pain at the office as long as I have to work on the mouse'', ''I can no longer garden, cook or even wash my plate'', ''It wakes me up at night and in the morning my elbow is completely stiff'' and a host of other complaints related to epicondylitis.
But what is epicondylitis?
In medical jargon, the suffix -'itis' denotes inflammation. Inflammation of the bronchi: bronchitis. Inflammation of the tendons: tendonitis. Inflammation of the conjunctiva of the eye: conjunctivitis! And so epicondylitis is an inflammation of the epicondyle!
So what is the epicondyle? A little anatomy is in order.

The elbow is the junction area, or simply the joint made up of the lower part of the arm bone, the humerus; of the upper part of the two bones of the forearm, notably the Ulna (Cubitus) and Radius. At the level of the lower part of the humerus, there are inside and outside two bony prominences called respectively: the medial epicondyle (internal) and the lateral epicondyle (external). These two prominences are easily palpable: they constitute “the bones” of the internal and external surfaces of the elbow. A large number of forearm muscles are inserted into each of the epicondyles, the majority of which are dedicated to the wrist or fingers. The bone surface being small, it is therefore understandable that the bulk of the shocks absorbed by the hand or the wrist will be transmitted and collected at the level of the epicondyle. As a result, we also understand that the epicondyle, whether internal or external, is therefore a zone of convergence of forces, and therefore a zone at risk.
The wrist and finger extensors are inserted into the lateral (external) epicondyle. Inflammation at this level is therefore called lateral epicondylitis, otherwise famously known as ''Tennis elbow''.
The wrist and finger flexors are inserted into the medial (inner) epicondyle. Inflammation at this level is therefore called medial epicondylitis, otherwise famously known as ''Golfer's Elbow''.
So what is causing this?
The causes of epicondylitis are many and many. The most common cases are:
– The work of tightening in rotation of the forearm.
– Exposure of the hand and upper limb to constant vibrations (handling machines, jackhammers, etc.).
– Physical work coupled with shocks (work with a hammer, punches, etc.).
– Bad posture, especially at the computer.
– Direct shocks, trauma or injury (as in an arm-wrestling challenge).
– Overload and poor movement in sport, poor technique and equipment (Weightlifting without good form or recovery, heavy racket, repeated movements with poor form, etc.).
– Nutrition poor in minerals, complete proteins and especially lack of good hydration.
– Mechanical problems in the neck or shoulder.
To these causes we add problems in the chemistry and biology of the body, such as in the case of certain diseases, the use of certain medications and other conditions that go beyond the epicondylar tendons themselves. These causes are not addressed by this article.
Solutions?
Fortunately, there are plenty of them!
Apart from the medical treatment prescribed by the doctor, other complementary care is very effective in solving this problem, in particular the physiotherapy!
Indeed, this treatment modality in manual therapy will act on muscular tensions, to seek to release them. It will also address all of the muscles upstream and downstream of the elbow if necessary, which can go from the neck to the hand! The physiotherapist will determine the areas to be treated after a postural observation and a series of palpations which will provide him with the necessary information to guide him in his approach. Massages, fasciatherapy, passive mobilizations, muscle tension lifting techniques, postural correction advice and stretching and exercises as needed, will be provided by the Physiotherapist to better help the client manage their symptoms and to correct the factors that caused the impairment.
Physiotherapy can also be combined with acupuncture and osteopathy which will help restore a more complete physical balance to both accelerate the recovery process and prevent recurrence of the disorder.
Do you think you have this condition? Don't forget to consult your doctor for a diagnosis and have yourself taken care of by care that will make your life easier!
Patrick P. Georgevitch
Physiotherapist – Trainer – Teacher